What Is Recurrent Corneal Erosion?
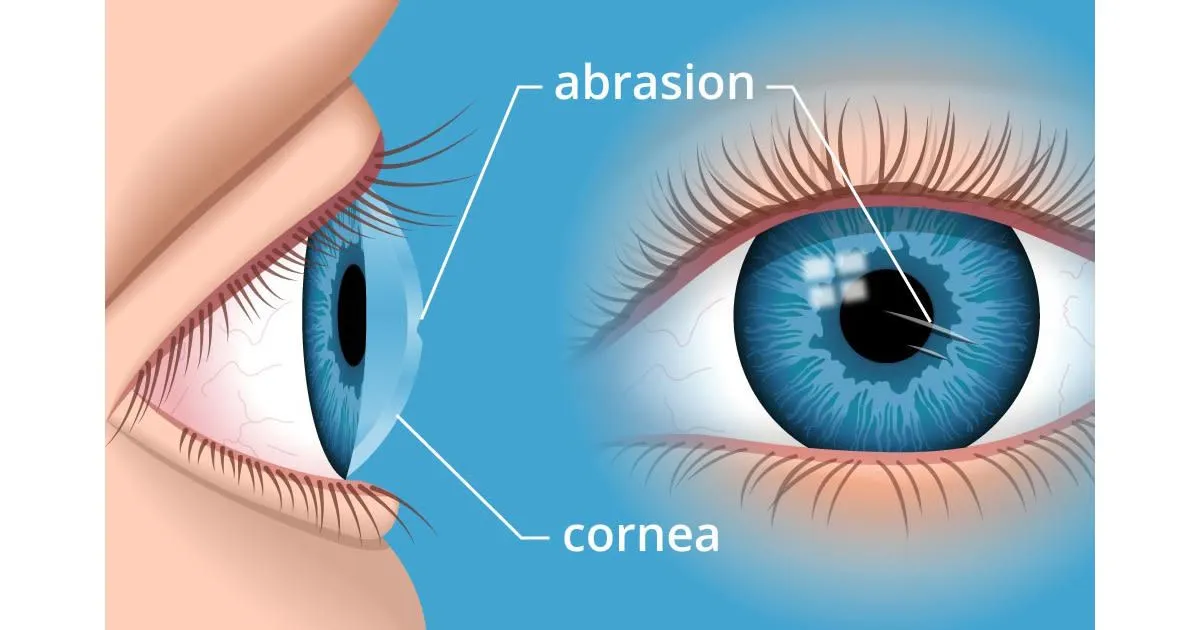
A corneal erosion or abrasion occurs when there is loss of the corneal epithelium, the cornea’s outer layer. These can occur if your cornea is scraped or injured, often leading to eye pain or other symptoms. There are 3 major causes of recurrent corneal erosion, which are:
- Previous corneal injury (corneal abrasion).
- Corneal dystrophy (map dot fingerprint dystrophy) – (abnormal structure changes of the cornea).
- Underlying corneal disease.
Who’s at risk?
The most likely victim of recurrent corneal erosion is the person who has had a previous corneal abrasion that was very sharp, clean, and linear, like that from a paper cut. Because the cut is so sharp, without ragged edges, it is less likely to stick down tightly to the underlying basement membrane. Think of gluing two pieces of wood together: if they are exceptionally smooth, they might not adhere as well as if the surfaces were rough. Those who have an abnormal structure to the corneal epithelium (called map-dot-fingerprint dystrophy) are at much greater risk of poor healing following a corneal abrasion and, thus, can develop recurrent corneal erosion.
Signs and Symptoms
Just as it is nearly impossible to see a corneal abrasion with the naked eye, the same is true for recurrent corneal erosion. What is most important is the time course. In recurrent corneal erosion, the patient can remember having had a corneal abrasion relatively recently (usually within the past 3–10 days) and then, most often when first opening the eye in the morning, feels a sudden burst of pain accompanied by symptoms of a corneal abrasion, which are:
- Lots of watery tearing
- Sensitivity to light (especially bright light)
- Blurry vision
- Redness of the eye
- Spasm of the muscles surrounding the eye resulting in squinting
- Feeling that something is in the eye
- Pain
These symptoms may not necessarily mean that you have a corneal erosion or abrasion. However, if you experience one or more of these symptoms, contact your ophthalmologist for a complete exam. These painful conditions commonly arise after a poke from a finger, tree limbs and bushes, or vigorous rubbing of the eye. Sometimes they are caused by contact lenses or other foreign bodies in the eye.
Tests and Diagnosis
Detecting an erosion or abrasion requires the use of fluorescein dye, which highlights the injured tissue during an eye exam. If present, underlying corneal disease also can be diagnosed during an eye exam. Special imaging or other testing is usually not necessary.
Treatment and Drugs
A corneal erosion or abrasion typically heals quickly, often within a few days to a week. It is important not to rub your eye during the healing process as the new epithelial cells are fragile and can easily be rubbed off. Sometimes your ophthalmologist may choose to patch your eye tightly. This facilitates healing of the damaged corneal epithelium and also reduces pain by preventing the blinking eyelid from irritating the affected area. Since both eyes move together and the eye is most painful when it moves, it is often helpful to rest the other eye as well.
Your ophthalmologist may recommend an antibiotic to prevent infection. Anesthetic drops can relieve pain and facilitate examination but may keep the eye from healing properly if used repeatedly. Anesthetic drops should never be used as a treatment. Long after an abrasion has healed it may spontaneously recur, and is often noticeable upon awakening in the morning. Recurrent corneal erosions often require repeat patching or the use of ointments at bedtime. Sometimes a soft or bandage-type contact lens is used to facilitate healing. Occasionally, treatment of the corneal surface with minor surgery is necessary to prevent recurrences.
If bacteria get into the tissues under the protective corneal epithelium, infection or a corneal ulcer can result. These complications can be very serious and cause loss of vision. Proper care by you and your ophthalmologist are necessary to help prevent serious consequences.
Contact SightMD today to schedule an appointment with one of our doctors to discuss your vision health at one of our convenient locations!


