What is Glaucoma?
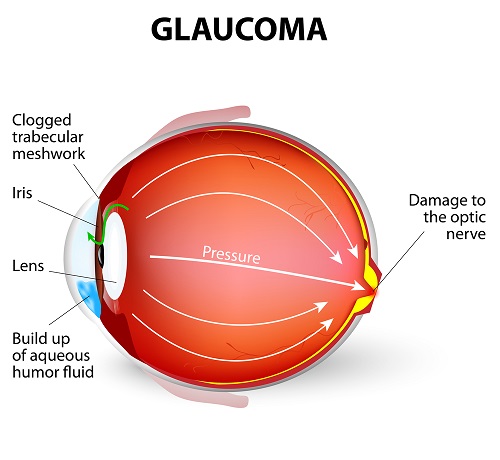
Glaucoma is an eye condition where the optic nerve becomes damaged, usually due to high pressure inside the eye. This damage can lead to gradual loss of vision, starting with peripheral vision and potentially progressing to blindness if left untreated.
Glaucoma, commonly called “the silent thief of sight”. Damage to or excessive pressure on the optic nerve and nerve fibers that form parts of the retina are the main causes of glaucoma. Typically this disease has no symptoms in its early stages. Over time if left untreated it can lead to blindness. According to the National Eye Institute, nearly 2.2 million Americans aged 40 and older have the most common form of glaucoma (open-angle glaucoma). Almost half of these people are not even aware they have the disease!
What are the Different Types of Glaucoma?
There are several different types of glaucoma, but the two major types are :
- Primary Open Angle Glaucoma (POAG)
- Closed Angle Glaucoma, or Angle-Closure Glaucoma
Primary open angle glaucoma is the most common form of glaucoma. With primary open angle glaucoma, inner eye pressure rises as the canals that drain fluid from the eye become clogged. POAG can develop over several years. Over time it can reduce vision if it is not diagnosed and treated. Angle-closure glaucoma occurs less frequently than POAG and is much more serious. With this form of the disease, eye pressure rapidly increases to high levels before draining. This overtime causes damage to the optic nerve. Closed angle glaucoma is an emergency and needs immediate medical attention.
What is the Difference Between Open and Closed Angle Glaucoma?
Primary open angle glaucoma does not cause any significant symptoms. Many people do not realize they have glaucoma until they start noticing vision loss at a later stage. At that point, any vision loss cannot be recovered. Therefore, we encourage routine eye examinations. Yearly glaucoma tests can help prevent glaucoma-related vision loss.
Closed-angle glaucoma is different. Because of the sudden increase in IOP, closed-angle glaucoma can cause significant symptoms as described below.
What are the Symptoms of Glaucoma
Differentiating between early and late-stage symptoms of glaucoma is crucial for early detection and management of the condition. Glaucoma is often asymptomatic in its early stages, which is why regular eye exams are essential for early detection. Its very important to understand that as the condition progresses, symptoms may become more noticeable. Here’s a breakdown of early and late-stage symptoms:
Early Stage Glaucoma Symptoms:
- No Symptoms: In many cases, glaucoma does not cause noticeable symptoms in its early stages. The condition may only be detected through routine eye exams, which include measurements of intraocular pressure and evaluation of the optic nerve.
- Mild Blurred Vision: Some individuals may experience mild blurring or haziness in their vision, particularly in the peripheral (side) vision. However, this symptom is often subtle and may not be noticed by the individual.
- Patchy Blind Spots: Glaucoma can cause the development of patchy blind spots in the peripheral vision. These blind spots may not be noticeable unless specifically tested during an eye exam.
Late Stage Glaucoma Symptoms:
- Severe Vision Loss: As glaucoma progresses, the peripheral vision loss may become more pronounced, leading to significant visual impairment. Individuals may develop tunnel vision, where only a small area of central vision remains intact.
- Difficulty Seeing in Low Light: Individuals with advanced glaucoma may have difficulty seeing in low light conditions or may notice halos or rings around lights, particularly at night.
- Eye Pain and Headaches: In cases of acute angle-closure glaucoma, which is less common but can be a medical emergency, individuals may experience sudden and severe eye pain, along with headaches, nausea, and vomiting.
- Redness and Swelling of the Eye: Glaucoma can sometimes cause redness and swelling of the eye, especially if there is increased pressure within the eye or if there are other complications such as inflammation.
Late-stage symptoms of glaucoma can significantly impact vision and quality of life making regular eye exams are crucial for early detection and treatment of glaucoma, even in the absence of symptoms. Early diagnosis and appropriate management can help preserve vision and prevent further progression of glaucoma.
How is Glaucoma Diagnosed?
There are many ways that an ophthalmologist can diagnose glaucoma. At SightMD, we are dedicated to providing thorough and precise diagnoses of glaucoma to ensure the preservation of our patients’ vision. Our experienced ophthalmologists utilize a range of advanced diagnostic techniques to accurately identify glaucoma and tailor treatment plans to each individual’s needs.
Tonometry
One of the primary methods we use to diagnose glaucoma is tonometry, which measures the pressure inside the eye, known as intraocular pressure (IOP). Elevated IOP is a significant risk factor for glaucoma, as increased pressure can damage the optic nerve over time. By accurately measuring IOP, our ophthalmologists can assess the risk of glaucoma and initiate appropriate interventions to manage the condition.
Optic Nerve Evaluation
A thorough evaluation of the optic nerve is essential for diagnosing glaucoma early and effectively . Our specialists utilize advanced imaging techniques such as optical coherence tomography (OCT) to assess the structure and health of the optic nerve. OCT provides high-resolution images of the optic nerve head, allowing our ophthalmologists to detect early signs of damage and monitor changes over time.
Visual Field Testing:
Visual field testing is another vital component of glaucoma diagnosis. This test assesses the full extent of a patient’s peripheral vision, which is typically affected in glaucoma. By measuring visual field loss, our ophthalmologists can determine the severity of the condition and track changes in vision over time. Visual field testing is crucial for monitoring glaucoma progression and guiding treatment decisions to preserve as much vision as possible.
Comprehensive Eye Exams:
In addition to specialized diagnostic tests, comprehensive eye exams are an integral part of glaucoma diagnosis at SightMD. During these exams, our ophthalmologists thoroughly evaluate the health of the eye, including the optic nerve, retina, and other structures. We also assess other risk factors for glaucoma, such as family history and medical conditions, to provide personalized care and early intervention.
What are the Treatment Options for Glaucoma?
At SightMD, we offer a comprehensive range of treatment options for glaucoma aimed at effectively managing the condition and preserving our patients’ vision. Our experienced ophthalmologists tailor treatment plans to each individual’s unique needs, considering factors such as the severity of glaucoma, medical history, and lifestyle preferences.
Surgical Glaucoma Treatment
We offer a range of surgical treatment options for glaucoma aimed at effectively managing the condition and preserving vision, particularly for patients with advanced or uncontrolled glaucoma. Our experienced ophthalmologists carefully assess each patient’s specific needs and medical history to determine the most appropriate surgical approach. The most common type of surgical treatment for glaucoma are:
- Trabeculectomy is a traditional glaucoma surgery that involves creating a small drainage flap in the sclera (the white part of the eye) to allow excess fluid to drain out, thereby lowering intraocular pressure (IOP). This procedure is typically performed in an operating room under local anesthesia and may require post-operative care and monitoring.
- Glaucoma Drainage Devices also known as tube shunts or aqueous shunts, are small implants placed in the eye to create a new drainage pathway for excess fluid. These devices are often used in cases where trabeculectomy has failed or is not suitable. Our ophthalmologists carefully select and place the appropriate drainage device based on each patient’s specific needs.
- Minimally Invasive Glaucoma Surgery (MIGS) encompasses a range of surgical procedures that offer a less invasive alternative to traditional glaucoma surgery. These procedures aim to improve the eye’s natural drainage system with minimal tissue disruption, resulting in lower IOP. MIGS procedures are typically performed in-office or as outpatient procedures and may include techniques such as trabecular micro-bypass stents or micro-pulse laser trabeculoplasty.
- Cyclophotocoagulation is a laser procedure that targets and reduces the production of aqueous humor (fluid) in the eye, thereby lowering IOP. This procedure may be recommended for patients with refractory glaucoma or those who are not candidates for other surgical interventions.
Non-Surgical Glaucoma Treatment
In addition to the surgical treatments we offer a range of non-surgical treatment options for glaucoma aimed at effectively managing the condition and preserving vision. These non-surgical approaches may be suitable for patients with early-stage glaucoma or those who prefer to explore conservative treatment options before considering surgery. The most common type of non-surgical treatment for glaucoma are:
- Medicated eye drops are often the first-line treatment for glaucoma. These drops work to lower intraocular pressure (IOP) by either reducing the production of aqueous humor (fluid) in the eye or increasing its drainage. Our ophthalmologists carefully select the most appropriate eye drops based on each patient’s specific needs and medical history.
- Laser procedures such as selective laser trabeculoplasty (SLT) or laser peripheral iridotomy (LPI), can help improve the drainage of fluid from the eye, thereby lowering IOP. These procedures are minimally invasive, performed in-office, and generally well-tolerated by patients.
- Oral medications may be prescribed to help lower IOP and manage glaucoma in some cases. These medications may work by reducing fluid production in the eye or improving its drainage. Our ophthalmologists carefully consider factors such as potential side effects and drug interactions when prescribing oral medications.
- Regular monitoring of IOP and glaucoma progression is essential for optimizing non-surgical treatment outcomes. Our ophthalmologists closely monitor patients’ eye health and response to treatment, making adjustments as necessary to ensure effective management of the condition and preservation of vision.
What Affects the Cost of Glaucoma Surgery?
Total treatment cost varies from patient to patient. The cost of your glaucoma surgery will depend on a variety of factors, including:
- Surgical method your doctor recommends
- Type of anesthesia used
- Medications you receive before or after your procedure.
Your doctor will discuss the cost of your procedure in detail during a consultation. Typically, most glaucoma procedures are covered under insurance.
What are the Risk Factors of Glaucoma?
- Age: Anyone who is over the age of 60 is at risk for glaucoma. The occurrence of glaucoma increases with age in all ethnic groups.
- Family history: Anyone who has a relative, such as a sibling or parent, who suffers from glaucoma is at higher risk.
- High intraocular pressure: People with elevated intraocular pressure are at a higher risk for glaucoma.
- Ethnicity: African Americans are at increased risk for glaucoma, especially after the age of 40.
- Diabetes: People who suffer from diabetes are at a higher risk of having glaucoma.
FAQs about Glaucoma Treatment
Glaucoma can indeed lead to blindness if left untreated or inadequately managed. As glaucoma progresses, it can cause irreversible vision loss, starting with peripheral vision and eventually leading to tunnel vision and, in severe cases, complete blindness. Early detection and proper management through regular eye exams, medication, laser therapy, or surgery can significantly reduce the risk of vision loss and help preserve eyesight.
Glaucoma, unfortunately, is not curable in the traditional sense meaning that once vision loss occurs due to glaucoma, it is irreversible. With early detection and appropriate treatment, the progression of the disease can often be slowed or halted helping to preserve the remaining vision and preventing further damage. Treatment options such as prescription eye drops, laser therapy, minimally invasive glaucoma procedures, and, in some cases, traditional glaucoma surgery can effectively manage intraocular pressure and help control the condition.
While there is no guaranteed way to prevent glaucoma, several proactive measures can help reduce the risk of developing the condition or slow its progression. Regular eye exams are crucial for early detection and treatment, allowing for timely intervention to help manage the disease effectively. Additionally, maintaining a healthy lifestyle, including regular exercise and a balanced diet rich in fruits and vegetables, can support overall eye health. Avoiding smoking and managing conditions such as diabetes and high blood pressure can also contribute to reducing the risk of glaucoma.
Engaging in regular exercise, such as brisk walking or aerobic activities, can help improve blood flow to the optic nerve and regulate intraocular pressure. Additionally, maintaining a healthy diet rich in fruits, vegetables, and omega-3 fatty acids can provide essential nutrients that support eye health. It’s also important to avoid smoking and limit caffeine intake, as both can increase intraocular pressure. Managing stress through relaxation techniques like meditation or yoga may also be beneficial, as stress can temporarily elevate intraocular pressure. Lastly, adhering to prescribed medications, attending regular eye exams, and following treatment plans recommended by healthcare providers are crucial for effectively managing glaucoma and preserving vision.
At SightMD, our commitment to excellence in glaucoma diagnosis and treatment ensures that our patients receive the highest standard of care for their vision health. We strive to preserve vision and enhance quality of life for individuals affected by glaucoma. For more information about Glaucoma please reference the American Academy of Ophthalmology’s post for further discussion on Glaucoma Symptoms, Causes, Diagnosis and Treatment. on Schedule an appointment with one of our experienced ophthalmologists today to take the first step towards preserving your vision for years to come.

Glaucoma Awareness Month: January Tips to Protect Your Sight
January Is Glaucoma Awareness Month: Understanding the “Silent Thief of Sight” January is Glaucoma Awareness Month, a dedicated time…

Top Eye Care Innovations of the Last Decade
How Technology is Reshaping Vision Care At SightMD, we believe that embracing the latest innovative eye care technologies—from AI…

Common Drugs That Can Worsen Glaucoma
Common Drugs That Can Worsen Glaucoma Glaucoma is a group of eye conditions that damage the optic nerve. This…