What is Uveitis?
Uveitis is inflammation inside your eye. Inflammation usually happens when your immune system is fighting an infection. Sometimes uveitis means your immune system is fighting an eye infection — but it can also happen when your immune system attacks healthy tissue in your eyes. Uveitis can cause problems like pain, redness, and vision loss.
Uveitis damages the part of the eye called the uvea — but it often affects other parts of the eye, too. Sometimes uveitis goes away quickly, but it can come back. And sometimes it’s a chronic (long-term) condition. It can affect 1 eye or both eyes.
Uveitis can cause vision loss if it isn’t treated — so it’s important to see your eye doctor right away if you have symptoms.
What are the Types of Uveitis?
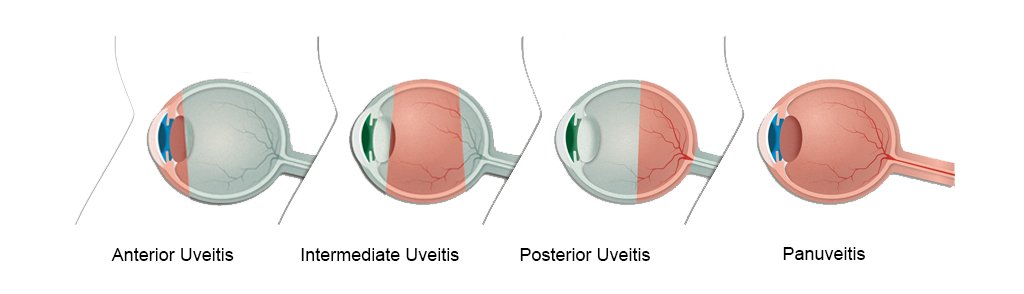
Different types of uveitis affect different parts of the eye.
- Anterior uveitis affects the iris at the front of the eye. It’s the most common type, and it’s usually less serious.
- Intermediate uveitis affects the ciliary body and the vitreous (gel-like fluid that fills the eye).
- Posterior uveitis affects the retina and the choroid at the back of the eye.
- Panuveitis affects all parts of the uvea, from the front to the back of the eye.
How to Recognize Uveitis?
The symptoms are like many other eye disorders, making it difficult to distinguish uveitis from other eye problems. Symptoms can include:
- Loss of vision
- Light sensitivity
- Swelling
- Redness
- Floaters
- Eye pain
Common Causes of Uveitis
Our body’s immune system uses inflammatory responses to fight several issues. From foreign invaders like bacteria to toxins we personally ingest, like alcohol, inflammation is a normal physical response used to process, kill, or drive out toxins, viruses or bacteria. However, when inflammation to something within the sensitive eye area occurs, uveitis may follow suit. The inflammatory response within the eye may be triggered by the following things:
- Autoimmune issues. When the immune system doesn’t function properly and begins attacking itself, the body has ceased working normally and can cause numerous issues. Lupus, Sjogren’s syndrome, hyperthyroidism and other autoimmune diseases can all cause issues to appear throughout the body, including in the eyes.
- Injury. If you’ve suffered a bruise or laceration from an eye or face injury, inflammation would be the body’s typical response to heal that area. This could cause acute uveitis that would most likely clear up on its own as the injury subsides.
- Infection. It’s no secret that we exist amongst millions upon millions of bacteria and viruses. When any one of these works its way into the eye, we can experience uveitis as the body attempts to clear it.
- Toxins. If topical ointments, make-up or other products work their way past our eye lashes into the eye, uveitis may develop as a response to attempting to clear out toxins.
- Unknown. It is more common that many cases of uveitis have unknown causes.
When to See a Doctor for Uveitis
Having an established medical history with your eye doctor is important in the diagnosis of uveitis. Regardless of if the eye condition is chronic or acute, it’s important that your ophthalmologist have a good understanding of your eye history and development over time.
Lab tests may first be conducted to rule out autoimmune diseases, bacterial or viral infections or other eye problems.
Diagnostic tactics for uveitis include:
- A routine eye exam and visual acuity test. Your ophthalmologist may first test your overall eye ability with a routine eye exam in which you read letters on a chart. This simple exam takes place at the ophthalmology office and allows your eye doctor to compare current results with your eyesight history to consider if your vision has been affected.
- Funduscopic examination. Your ophthalmologist will start by widening the pupil with a dilating liquid. Then, he or she will use a microscope to look through the pupil to the back of the eye to look for any inflammation or damage.
- Ocular pressure test. This test is also used frequently in routine eye examinations to test for glaucoma. A tonometer measures pressure in the eye by blowing puffs of air into it. Depending on your eye sensitivity, eye drops may be used to numb the area.
- Silt Lamp Examination. Typically, a dye is used to temporarily stain the eye and color the blood vessels for ease of inspection. Then, a silt lamp is used to magnify and illuminate the front portion of the eye to see if inflammatory cells exist.
- Blood test. If your doctor suspects the uveitis is caused by an underlying issue, they may order a blood test to rule out possible STIs or other infectious causes.
Uveitis Treatment
Medicines called steroids can reduce inflammation in your eye. This can ease symptoms and prevent vision loss. Your eye doctor may prescribe steroids in a few different ways:
- Eye drops. Prescription eye drops are the most common treatment.
- Pills. Your eye doctor may also prescribe steroids as a pill.
- Injections. In some cases, your eye doctor might put the steroid in or around your eye with a small needle.
- Implants. If other treatments don’t work, your doctor might suggest surgery to put a small device called an implant into your eye. The implant gives you regular small doses of the steroid over time.
Steroids can have side effects and can increase your risk for cataracts and glaucoma. If you take steroids for uveitis, it’s important to get regular eye exams to check for signs of these problems.
Your treatment plan will depend on several factors — like which part of your eye is affected, and other health conditions you have. For example, your doctor may prescribe medicines to help control your immune system. You can work with your doctor to find the right treatments for you.
Contact SightMD today to schedule an appointment with one of our doctors to discuss your vision health at one of our convenient locations!
Flashes and Floaters: When Are They an Eye Emergency?
Changes in vision, such as flashes of light or floaters, can be unsettling. While these symptoms are often benign,…
Understanding Laser Surgery for Retinal Tear
What to Expect During Recovery after Laser Surgery for Retinal Tear Laser surgery for a retinal tear is a…
Understanding what Age-Related Macular Degeneration is
Age-related macular degeneration (AMD) is the most common cause of vision loss in individuals over the age of 50….