Cataract Surgery – The Complete Guide By SightMD
Cataract surgery is a procedure that can significantly enhance your vision and overall quality of life. At SightMD our advanced facility specializes in delivering personalized and cutting-edge cataract surgical services tailored to your specific requirements.
Our skilled surgeons use modern technology to help you at every stage. They ensure that your experience is easy and comfortable. Discover how SightMD’s cataract surgery services can improve your vision and bring clarity to your world.
What are Cataracts?
Cataracts develop when proteins clump together, causing opacity in the eye’s natural lens. This eye condition is most common in individuals aged 55 and above and progresses slowly over time. Luckily, cataracts can be treated through routine surgery.
Opting for cataract surgery can help restore clear vision while enhancing your quality of life. The suitable treatment for you will depend on the severity of your vision impairment.

How do Cataracts Form?
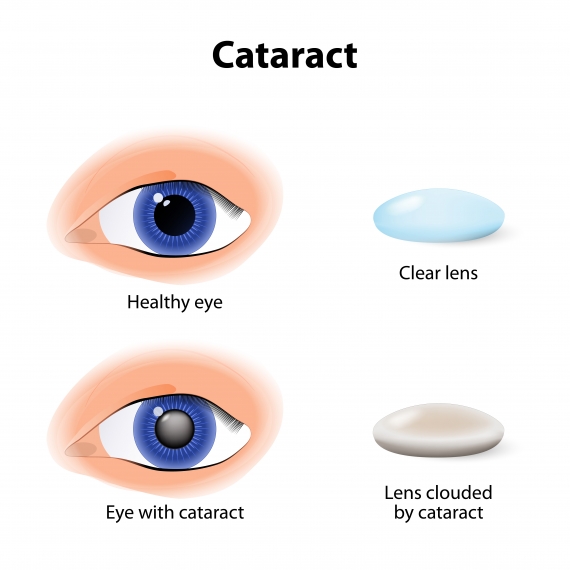
Cataracts form when proteins clump together, causing cloudy natural lens spots in the usually clear lens part of the eye. This leads to blurred vision as some of the incoming light is blocked from reaching the retina. Most often people may notice glare from sunlight during the day and from headlights while driving at night. This clustering process typically occurs slowly and does not cause any pain.
What Are The Symptoms of Cataracts?
Since cataracts develop slowly, the symptoms may not be immediately noticeable. Overtime you might even adapt to them as your vision worsens. Early detection allows us to explore treatment options and can help delay the progression of the condition.
If you experience any vision impairment, you should seek a diagnosis. Typical symptoms of cataracts include:
- Blurred or cloudy vision
- Muted colors
- Lack of definition
- Glare or the appearance of halos around light sources
- Inhibited night vision
- Double vision
- A marked degradation in your visual prescription over time (for eyeglass users)
How can Cataracts be Prevented?
As we age, the likelihood of developing cataracts increases. Currently, there is no proven method to prevent cataracts. However, there are strategies that may help reduce the risk of developing them. Wearing sunglasses and hats outdoors can protect your eyes from UV rays, which can prevent cataracts by stopping the breakdown of proteins.
To slow down cataracts formation, try quitting smoking and following a well balanced diet. Regular eye check-ups can aid in early detection of cataracts. If a cataract is found early, vision can be improved without surgery using glasses or more indoor light.
How are Cataracts Diagnosed?
A cataract exam may require a combination of tests to gauge not only if you have cataracts, but the severity of the cataracts. Doctors may use further testing beyond this to determine what type of cataract you have.
A cataract exam checks for cataracts and their severity. During the exam your doctor may do more tests to determine exactly what type of cataract you have. Cataracts are common as people age, especially in those over 55. Risk factors include eye injuries, family history, smoking, and some medications.
When Should Cataracts be Removed?
A cataract may not need immediate removal if it does not significantly affect your lifestyle. Sometimes, enhancing your vision can be as easy as adjusting your eyeglass prescription. A common misconception that a cataract must be fully developed before it can be removed.
However, once diagnosed with a cataract, regular vision monitoring is crucial to identify any changes. If a cataract begins to cause vision problems that interfere with your daily activities, cataract surgery may be required.
How are Cataracts Removed?
When detected early, vision can improve with corrective lenses. If these measures do not help, doctors may suggest surgical removal of the cataract. If left untreated, the cataract may progress. At SightMD, our doctors specialize in advanced cataract surgery.
Thanks to cutting-edge technology, our cataract procedure typically lasts between 10 to 20 minutes. Patients can return home on the same day. The two most common types of surgery are:
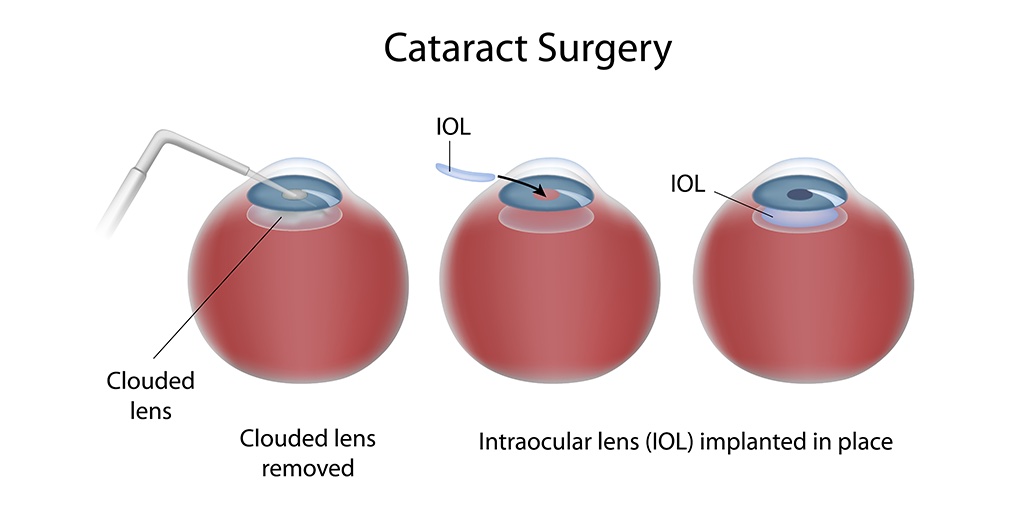
- Small-incision cataract surgery (Phacoemulsification) – Small-incision cataract surgery is the most common type of cataract removal. The eye surgeon makes a small opening on the eye, next to the outer corner. A tiny probe gives off ultrasound waves to dissolve the core, hard part of the cloudy lens. The rest of the cataract material is then removed by another probe, which provides suction through the same opening.
- Extracapsular surgery involves making a bigger opening in the eye to take out the hard center of the lens. The rest of the cataract material is then taken out by suction, through the large opening. This type of larger incision cataract surgery is rarely done today.
During surgery, the old lens is removed and replaced with a new artificial lens called an intraocular lens (IOL). This is done through the same opening. An IOL is a transparent, artificial lens that requires no maintenance. It integrates into the eye.
By using an IOL, an individual typically experiences improved eyesight as light can now reach the retina. The individual does not perceive or sense the presence of the new lens.
What to Expect after Cataract Surgery
After surgery, colors may appear brighter as the cloudy lens is removed. This change can be noticed within a few hours. However, your vision may be blurry during the first couple of days, and your eye may be slightly light-sensitive. Dryness, occasional itching, burning and/or red eyes are also common Most of these effects will end within a few days.
Your doctor will prescribe eye drops or medications to prevent or control inflammation, infection or high pressure of the eye. An eye shield is also recommended at bedtime to protect the operated eye.
You will also be scheduled for three or four follow-up appointments with your doctor to monitor your recovery progress. A month after the surgery, you will need an eye exam so you can be prescribed new eyeglasses if necessary.
How Long is Recovery from Cataract Surgery?
After undergoing cataract surgery, many patients typically return to work with light duties within two to three days. Nevertheless, complete recovery from the surgery usually spans from one to two months. This time period is when your eye adjusts to the new lens and your vision returns to its best level.
How Much Does Cataract Surgery Cost?
Without private insurance or Medicare, you can expect an out-of-pocket expense anywhere from $3,000 to $7,000 per eye. In most cases, insurance covers cataract surgery.
Medicare and most insurance companies deem cataract surgery medically necessary. This allows for most cases to cover the procedure. Some plans have deductibles and copays.
Patients are pleased to know that our cataract surgeons, anesthesiologist, and eye surgery center are covered.
What Factors Affect the Cost of Cataract Surgery?
The cost of cataract surgery can vary on such factors as:
- Setting: Having cataract surgery in an ambulatory surgical center tends to cost less than outpatient surgery in the hospital.
- Type of surgery: Two traditional techniques are phacoemulsification (“phaco”) and extracapsular cataract extraction surgery (ECCE). Phaco uses a small incision, while ECCE uses a larger incision. For these procedures, uninsured people can expect to pay $3,000 to $5,000. Laser-assisted cataract surgeries, with more advanced technology, can average $4,000 to $6,000.
- Type of lens: You and your doctor can choose the type of IOL that suits you best. The monofocal lens allows clear vision at one distance and is cheaper than the multifocal lens. The multifocal lens improves vision for both near and far distances.
- Surgeon experience: The technology used for phaco may require the surgeon to have more extensive medical training. As a result, this technique can be more costly than other types of cataract surgery.
- Post-surgical complications: Sometimes, the artificial lens can also become cloudy weeks or years after the surgery. Addressing the problem may call for a laser surgery known as posterior capsulotomy, which costs about $600 to $800.
Cataract Common FAQs
How long should I wait before I get cataract surgery?
Many people live with cataracts that do not impair their vision. We do not recommend surgery for these individuals. Generally, if your vision loss becomes significant enough to interfere with your daily activities, then we do recommend surgery.
Can cataracts return after surgery?
No, once removed a cataract cannot redevelop. However, a secondary cataract may develop around the IOL. Treatment for secondary cataracts consists of a simple, painless laser procedure. This procedure clears the fogged area around the lens.
Are there treatment options for cataract without surgery?
Yes, if caught early before the cataracts have significantly impaired your vision. Your eye doctor may be able to change your lens prescription to mitigate the development of cataracts. Beyond that, there is nothing that can treat a cataract without surgically removing it.
What are the risks of cataract surgery?
Despite advancements in cataract surgery, including laser treatment, it’s important to remember that all surgeries have risks. With that in mind, our experienced cataract surgeons have made cataract surgery a large focus of our practice. We have successfully performed this procedure on many individuals and our skilled surgeons use advanced technology to reduce risks.
Some of the potential complications of cataract surgery include:
- Posterior Capsule Opacity – a condition that can impair vision after cataract surgery
- Malpositioned/Dislocated Intraocular Lens
- Eye Inflammation
- Retinal Detachment
- Corneal Or Retinal Swelling
- Increased pressure inside the eye
- Bleeding or Infection inside the eye
- Ptosis
Contact SightMD to schedule an appointment with a doctor to discuss your vision at one of our convenient locations!

Cataract Surgery Risks & Downsides: What Patients Should Know
Is There a Downside to Cataract Surgery? Cataract surgery is one of the safest and most effective procedures in…

Can You Have Cataract Surgery Twice? Understanding Secondary Cataracts and YAG Laser Treatment
When Vision Becomes Cloudy Again Cataract surgery is one of the most common and successful procedures in modern medicine,…

“Blurry Vision” After Surgery?
What Happened to That “Blurry Vision” After Surgery? Long-Term Outcomes Explained Eye surgery—whether it’s cataract surgery or LASIK eye…